Why Real‑World Testing is Crucial in Getting Hospital 2.0 Right

The National Audit Office’s latest update on the New Hospital Programme (NHP) is a timely reminder of the scale of transformation underway across England’s healthcare estate, and of the critical importance of testing ideas in practice, not just on paper. The report makes clear that while the Programme is now on a more realistic footing, success depends on ensuring that the new standardised “Hospital 2.0” model genuinely works for the clinicians, patients and operational teams who will rely on it.
Real‑World Prototyping at Full Scale
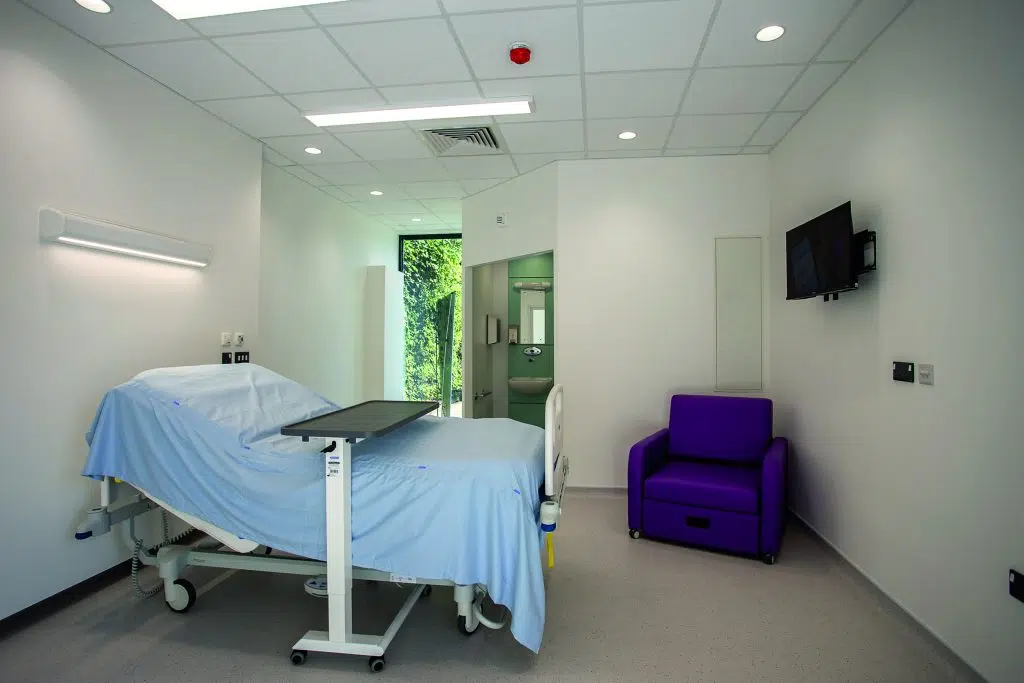
One of the most striking findings in the NAO report is the emphasis on real‑world prototyping. The NHP, in partnership with Reds10, constructed a full‑scale single‑bedroom prototype to identify opportunities to reduce space and cost, and to test whether staff could deliver care safely and effectively, including responding to cardiac arrest scenarios and supporting patients after a fall. At Reds10, we are proud to have enabled this essential testing environment. By creating a true‑to‑life, fully functional prototype, we provided NHS leaders and clinical teams with the ability to experience and interrogate the Hospital 2.0 concept at real scale.
Identifying Issues Early and Embedding Continuous Improvement
Critically, prototyping uncovers friction points early, long before they risk becoming ingrained into facilities that will serve communities for decades. The NAO highlights that while the Hospital 2.0 design has taken longer to develop than originally planned, ensuring the design is right is essential to achieving operational efficiencies, digital integration and improved patient experience. This is precisely why full‑scale testing is indispensable. The complexity of modern healthcare simply cannot be reduced to a design guide alone. It must be experienced, worked in and stress-tested.
NHP clinical teams and a wide range of stakeholders, including public and patient voice forums, reviewed and tested the prototype Reds10 delivered for months, validating observation from corridor to bedside, patient transfer from trolley to bed, assisted movement into the bathroom pod, bed manoeuvrability, response to emergencies such as crash calls, and recovery from falls. They have stress‑tested service accessibility in ceilings and pods, connection details at the corridor‑to‑bedroom interface, and the practicality of equipping choices, lighting, window types, and door swings.
The rigorous process of testing and extensive programme of stakeholder engagement led to multiple improvements to the original designs aimed at ironing out deficiencies identified through clinical feedback. We rebuilt some parts of the prototype five times in response to feedback to ensure each element is absolutely optimised from a clinical perspective.
Preparing for the Scale and Challenge of Hospital 2.0
The NAO’s findings also underscore the scale of the challenge. With schemes now expected to open later than previously planned, some by nearly a decade, the pressure is on to ensure that every design decision is robust, evidence‑based and capable of future adaptation. A standardised approach will only deliver value if it is informed by real user behaviour, clinical flow and frontline insight. Our prototype enabled exactly this kind of engagement, ensuring that trust leadership and clinical experts could feed back directly into the design.
Moreover, the Programme’s success relies not just on infrastructure but on shifts in clinical models, digital readiness and workforce practice. The NAO notes concern from some trusts that new designs may require more staff or new operating models, and that clinical buy‑in will be essential for achieving the intended benefits. Again, prototyping provides clarity. It gives clinicians a voice in shaping spaces and procedures, ensuring they feel confident, capable and prepared for the hospitals of tomorrow.
Building a Future Hospital Model That Works in Practice
As the NHS embarks on delivering 46 schemes over the next two decades, the importance of getting Hospital 2.0 right cannot be overstated. Standardisation offers huge potential but only if the design is proven, validated and adaptable.
Innovation only works when it’s tested by the people who use it. The NAO’s report reinforces that truth. At Reds10, we are proud to be helping the NHS build a future hospital model whose design is grounded in real clinical practice and tried, tested human experience.